October 16, 2009
Vaccine against flu: Distribution
If you think that all problems are solved after you have read all about the long vaccine production, you’re wrong. There is still the issue of distribution:
![]() As the vaccine manufacturing process is slow and continuous, it is not possible to produce enough doses for everyone. Nowadays, our yearly vaccine production is of 700 to 900 million at a maximum. In the case of an outbreak, changing the vaccine’s composition for a single extraction, as opposed to the three generally used, may imply a production two or three times larger, but still far from the necessary amount to immunize everyone. This may not even happen, considering that a single dose is enough for immunization. [1]
As the vaccine manufacturing process is slow and continuous, it is not possible to produce enough doses for everyone. Nowadays, our yearly vaccine production is of 700 to 900 million at a maximum. In the case of an outbreak, changing the vaccine’s composition for a single extraction, as opposed to the three generally used, may imply a production two or three times larger, but still far from the necessary amount to immunize everyone. This may not even happen, considering that a single dose is enough for immunization. [1]
This scenario gets worse by the nature of a pandemic virus. Instead of the seasonal virus, which is already known and followed up during the year, the pandemic virus has never been seen before. We can produce and store vaccines against seasonal flu even if the virus mutates, the odds of crossed immunity (immunity against the vaccine that attacks the new virus) are high.
In the case of pandemic virus, the chances of having the right vaccine stored are very low. Influenza A (H1N1) is not recognized by antibodies generated against the latest seasonal vaccines, although it is susceptible to those generated against the 1976 vaccine. It makes sense, since the 1976 vaccine was produced against a swine virus. [2]
That is why we can not rely on previous vaccines and we need to speed up in order to develop a vaccine against Influenza A (H1N1), and the same goes for the next pandemic virus appearance. We can develop the vaccine’s strainn and start production only after the virus appears, following up closely its mutations to certify that the vaccine will still generate protective immunity.
With doses production in a continuous flow, governments need to prioritize who must get them first. Here, a point must be made. In the case of a serious outbreak caused by a quite lethal Influenza, as it would be the case if a highly pathogenic H5N1 was to be efficiently transmitted between humans, everyone would need to be immunized under risk of death. But in the case of a pandemic virus as Influenza A (H1N1), which its main threat currently is the amount of people it may infect and not its severity, the immunization objective is to reduce the chances of spreading the virus.
For the Influenza to spread and live within a population the number of susceptible people must be quite large and they need to be in very close contact with each other since a person who contracts flu gets cured in about a week, and later is immunized against that virus strain. The flu “disappears” after winter because a large amount of people is already immunized, and favorable conditions for the spreading of the virus are over. Vaccine’s role is to break that chain.
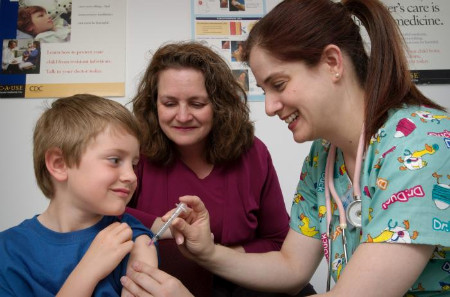
The vaccination priority is to guarantee that people that were exposed to risks have their health protected, as elders and health employees, and to undermine the virus transmission seedbeds. Hence it is important to immunize children at school age. They are instrumental to deter flu from spreading, at least according to the last transmission mathematical models. [3]
When a child that is going to interact with other children at school, parents or manipulate toys and get in touch with several objects and common spaces, is immunized the protection reaches not only the child but everyone around him. Imagine a housewife that gets a vaccine dose but is not supposed to get in touch with many people. She is a terminal point in the transmission chain, and only that point will be out of risk. When a child gets a dose, all points which will get in contact with the child will be more protected.
However, planning is not limited to distribution within one country. There is also the issue of granting poorer countries access to the vaccine. Flu’s vaccine is produced by few and huge private research centers, which charge for the doses. In the case of seasonal flu, demand for doses is quite lower than production-limit, once Influenza is not a big threat in many places, and the immunization focus are the most susceptible we have seen. But during an outbreak as we have now, all available doses are bought. The whole 2009 production is compromised.
How can poor countries have access to this, if in many places medicine costing dollar cents are not taken? Some laboratories have promised to distribute millions of doses for undeveloped nations, but the numbers are not even close to real necessity. The market rationale of giving more to those who pay more should not be applied to such an important topic as the protection against an outbreak. [4]
Finally, there is another delicate issue in immunization. Public’s acceptance. In addition of receiving and distributing vaccine doses as soon as possible, countries must ensure that their inhabitants will adhere to immunization. At this point, undeveloped countries are better prepared, for they are still preparing their large-scale immunization campaigns against a series of diseases which already have disappeared in richer nations.
Here, the role of making population conscious and clarifying questions is very important. Even more important since anti-immunization campaigns are getting stronger in the United States and are arising in Europe, as well as e-mails and websites that hold false information (that vaccine may kill or that it contains mercury, etc). We can not go through the whole process of producing, distributing and storing vaccines and fail at the last stage, which is to guarantee that all people in need of immunization are really immunized.
Source:
[1] Butler, D. (2009). Vaccine decisions loom for new flu strain Nature, 459 (7244), 144-145 DOI: 10.1038/459144a
[2] Hancock, K., Veguilla, V., Lu, X., Zhong, W., Butler, E., Sun, H., Liu, F., Dong, L., DeVos, J., Gargiullo, P., Brammer, T., Cox, N., Tumpey, T., & Katz, J. (2009). Cross-Reactive Antibody Responses to the 2009 Pandemic H1N1 Influenza Virus New England Journal of Medicine DOI: 10.1056/nejmoa0906453
[3] Medlock, J., & Galvani, A. (2009). Optimizing Influenza Vaccine Distribution Science, 325 (5948), 1705-1708 DOI: 10.1126/science.1175570
[4] Yamada, T. (2009). Poverty, Wealth, and Access to Pandemic Influenza Vaccines New England Journal of Medicine, 361 (12), 1129-1131 DOI: 10.1056/NEJMp0906972
La vacuna contra la gripe: Distribución
Si después de leer sobre la longa producción de la vacuna Ud. cree que todo se ha resuelto, está equivocado. Hay aún la dificultad de la distribución:
Como el proceso de fabricación de la vacuna es lento y continuo, no es posible producir dosis suficientes para todas las personas. Actualmente, nuestra producción anual de la vacuna contra la gripe estacional es de un máximo de 700 hasta 900 millones de dosis. En el caso de una pandemia, cambiar la composición de la vacuna para un linaje apenas, en vez de las tres en generalmente usadas puede significar en una producción dos o tres veces mayor, pero lejos aún del necesario para vacunar a todos. Esto al considerarse que solamente una dosis es suficiente para la inmunización, lo que puede no ser logrado. [1]
Esto empeora aún más por la naturaleza de un virus pandémico. Al contrario del virus estacional, que ya es conocido y seguido durante el año, el virus pandémico es inédito. Podemos producir y almacenar vacunas contra la gripe estacional, mismo que el virus mute las probabilidades de inmunidad cruzada (inmunidad contra la vacuna que ataca al nuevo virus) son altas.
En el caso del virus pandémico, las probabilidades de haberse almacenado la vacuna correcta son muy bajas. El Influenza A (H1N1) no es reconocido por los anticuerpos producidos contra las últimas vacunas estacionales, aunque sea susceptible a los producidos contra la vacuna del año 1976. Lo que hace sentido, pues la vacuna del año 1976 fue producida contra un virus porcino. [2]
Por eso, no podemos contar con vacunas previas y necesitamos apurarnos para desarrollar una vacuna contra el Influenza A (H1N1), y lo mismo debe repetirse con el aparecimiento del próximo virus pandémico. Podemos desarrollar el linaje de la vacuna y empezar la producción después que el virus aparece, siguiendo acerca las mutaciones del virus para asegurarnos de que la vacuna aún generará inmunidad protectora.
Con la producción de las dosis en flujo continuo, los gobernantes necesitan priorizar quienes deben recibir las dosis primero. Aquí se necesita clarificar algo. En el caso de una pandemia grave, causada por un Influenza muy letal, como sería el caso si el H5N1 altamente patogénico fuera transmitido eficientemente entre los humanos, todos precisarían ser vacunados bajo risco de muerte. Pero en el caso de un virus pandémico como el Influenza A (H1N1), cuyo peligro mayor es el número de personas que puede infectar, y no su severidad, el objetivo de la vacunación es reducir las probabilidades de contagio.
Una vez que una persona contrae gripe y se cura en aproximadamente una semana, y después está inmune a aquella cepa viral, para que el Influenza se propague y se mantenga en una población el número de personas susceptibles necesita ser muy alto y ellas necesitan estar en contacto muy cercano. La gripe “desaparece” después del inverno pues la mayoría de las personas ya está inmune y las condiciones favorables al contagio se las quitaron. El rol de la vacuna es lo de romper esta cadena.
La prioridad en la vacunación es la de garantizar que las personas bajo riesgo mayor tengan la salud garantizada, por ejemplo viejos y empleados de salud, y minar los focos de transmisión del virus. De ahí la importancia de vacunar niños en edad escolar. Ellos son la clave para quitar la propagación de la gripe, por lo menos según los últimos modelos matemáticos de transmisión. [3]
Cuando un niño que va a convivir con otros niños en la escuela, con los padres, manipular juguetes y tener contacto con muchos objetos y espacios comunes, recibe la vacuna, no solamente él estará protegido sino que todos alrededor. Considere un ama de casa que no tiene contacto con muchas personas durante la semana recibiendo una dosis de la vacuna. Ella es un punto terminal en la cadena de transmisión y solamente este punto estará fuera de riesgo. Cuando un niño recibe la vacuna, todos los puntos con los cuales él va tener contacto estarán más protegidos.
Pero la planeación no se limita solamente a la distribución dentro de un país. Hay también la cuestión del acceso de los países más pobres a la vacuna. La vacuna contra la gripe es producida por pocos y grandes centros de investigación privados, que cobran por las dosis. En el caso de la gripe estacional, la demanda por las dosis es inferior a la producción límite, una vez que muchos lugares no tienen el Influenza como una gran amenaza y el foco de vacunación son los más susceptibles que hemos visto. Pero durante una pandemia, como la de ahora, todas las dosis disponibles son compradas. Toda la producción del año 2009 ya está comprometida.
¿Cómo países pobres pueden tener acceso a esto, si en muchos lugares remedios que cuestan centavos de dólar no son tomados? Algunos laboratorios se han comprometido a repartir millones de dosis para países no desarrollados, pero los números no llegan cerca de la real necesidad. La estrategia de mercado de quien paga más recibe no debe aplicarse a una cuestión tan importante como la protección contra una pandemia. [4]
Por fin, hay aún otro punto delicado en la vacunación. La aceptación del público. Además de recibir y repartir las dosis de la vacuna lo más rápido posible, los países necesitan garantizar que sus habitantes van a adherir a la vacunación. En este momento, los países subdesarrollados están más listos, pues están aún manejando campañas de vacunación en larga escala contra una serie de enfermedades que ya se erradicaron en países más ricos.
Aquí, el rol de dar consciencia a la población y quitar las dudas es muy importante. Aún más ante campañas anti-vacunación cada vez más fuertes en Estados Unidos y que están surgiendo en Europa, así como correos electrónicos y sitios propagando falsa información de que la vacuna puede matar o que contiene mercurio, etc. No podemos pasar por todo el proceso de producir, repartir y almacenar vacunas para fracasar en la última punta, garantizar que las personas que necesitan ser vacunadas lo sean en realidad.
2 Comments » Posted in: Uncategorized


[...] during some weeks of the year, the common flu season that lasts from 5 to 10 weeks. This is why the vaccination campaigns have to occur about one month in advance. Thus, there is enough time to produce immunity before the [...]
[...] monitoring of variants, biannual meetings to discuss which of them will be used in the vaccine, production cycles and periodic tests, etc. Moreover, there is the worst problem: the adherence to the vaccine. Every year people need to [...]